June 22, 2021
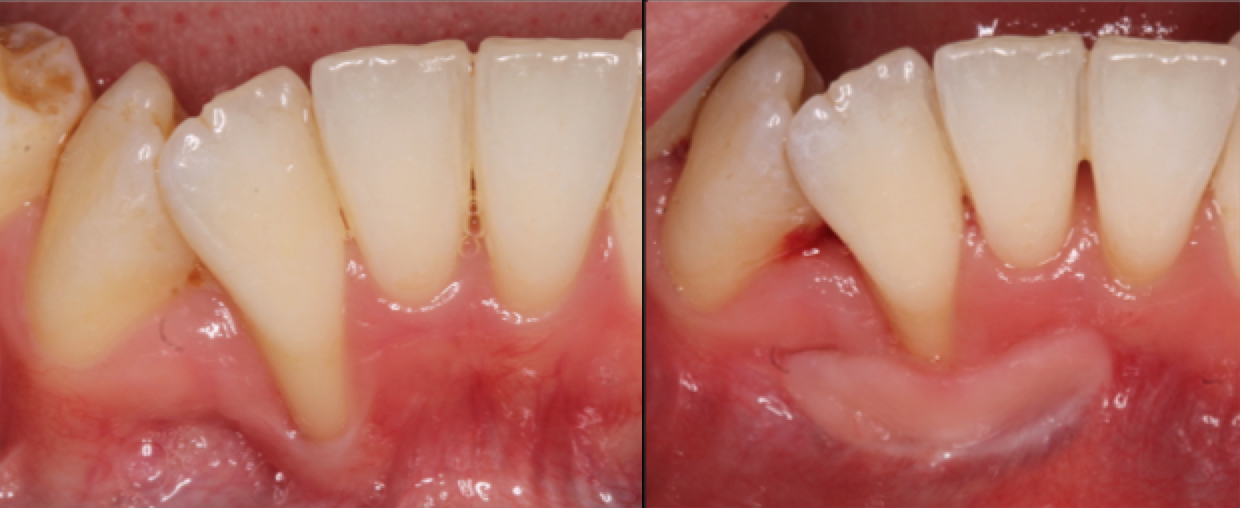
- Definition – Gingival recession can be defined as an apical shift of the gingival margin with exposure of the root surface to the oral cavity.
- Assessment – When assessing recession it’s important not only to measure the amount of recession but also consider the level of inflammation, width/shape of the recession defect, the amount of attached keratinised gingiva, depth of the sulcus, frenal attachments, biotype and bone levels. Photographs and study casts can also be helpful in keeping a record of recession.
- Aetiology – When understanding the causes of recession, it’s useful to split this up into predisposing factors and precipitating factors. Predisposing factors include: orthodontic movement of teeth to positions outside the labial/lingual alveolar plate, fenestrations/dehiscences and a thin biotype. Predisposing factors include trauma from overzealous toothbrushing/interdental cleaning, direct trauma from habits/piercings/malocclusion as well as inflammation (suboptimal plaque control).
- Classification – It can be helpful to classify it according to Miller’s classification (1985): Class I – marginal tissue recession that does not extent to the mucogingival junction and no loss of interdental periodontal attachment, Class II – marginal tissue recession that extends to or beyond the mucogingival junction and no loss of interdental periodontal attachment, Class III – marginal tissue recession that extends to/beyond the mucogingival junction with periodontal attachment loss in the interdental area or malpositioning of teeth, Class IV – marginal tissue recession that extends to/beyond the mucogingival junction with severe bone or soft tissue loss in interdental area and/or severe malpositioning of the teeth.
- Predictability – The classification helps to predict expected complete root coverage depending on the class and its relevant features. Class I and II – likely to get predictable root coverage in 100% of cases, Class III partial (50-70% cases) and impossible/very unlikely in Class IV (<10%).
- Consequences of recession – Be aware of the consequences of recession and ensure you explore these with your patient. Consequences may include: pain/sensitivity, poor aesthetics, inflammation and plaque retention (plaque control more difficult altered gingival architecture), root caries and abrasion.
- Initial aims of therapy – The initial aims of therapy for recession should include the management of the modifiable aetiology factors. This will involve ensuring adequate plaque control, addressing any overzealous brushing, desensitising roots etc.
- Indications for surgery – Aesthetics (patient demand), hypersensitivity, keratinised tissue augmentation, root abrasion/caries, inconsistency/disharmony of gingival margins and prevention of progression.
- Surgical procedures – The technique chosen depends on the clinical scenario and goals of treatment. For example, if it is a localised recession defect of the lower incisor following orthodontics, one may consider a free gingival graft to thicken the tissue (to prevent further recession and make oral hygiene procedures more comfortable). If it is a recession defect around an aesthetic site one may consider a root coverage procedure e.g. a coronally advanced flap, tunnelling or a rotational flap.
- Refer – If you’re unable to complete the surgical procedure yourself, ensure you refer to a periodontist in a timely manner.
Learn more by reading some of our other articles here.



