Home/Articles / General Dental / Reena’s Notes: Peri-implant Disease with Dr Mark Ide – 5 Common Questions
January 11, 2016
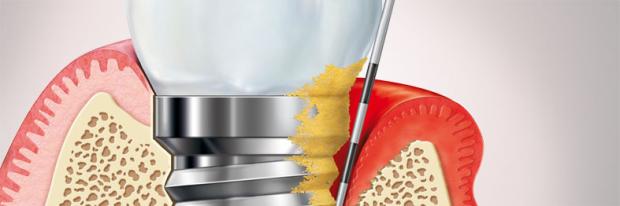
1. What do we know about peri-implant mucositis?
- Definition – a reversible inflammatory process in the soft tissues surrounding a functioning implant.
- Prevalence – bleeding on probing in 80% of implants (Lekholm et al 1986), 73% after 9-14 years (Roos-Jansaker et al 2006), 90% of implant sites (Fransson et al 2005).
- Cause – inflammation in response to marginal plaque.
- Signs & symptoms – marginal tissue swelling, bleeding on probing/suppuration, deeper probing depths, may be asymptomatic, soft tissue tenderness, bad taste/halitosis.
- Outcomes – continuation (stability)/peri-implantitis.
- Management – plaque control.
2. What do we know about peri-implantitis?
- Definition – an inflammatory process additionally characterised by irreversible loss of peri-implant bone surrounding a functioning implant.
- Prevalence – around 28% of patients (Frannson et al 2005), 43+% of patients after 9-14 years (Roos-Jansaker et al 2006).
- Cause – host response to plaque and secondary factors (may include cement and implant surface).
- Signs & symptoms – Bone loss with a saucer shaped/wedge shaped defect progressing down the implant, increased peri-implant pocketing, bleeding/suppuration after probing, fistula/sinus, marginal erythema/swelling, may be asymptomatic/painful.
- Outcomes – poor aesthetics, implant failure/loss, pain, recurrent infection.
- Management – referral!
3. What risk factors should be considered in the treatment planning, consent and maintenance aspects of patient care?
- Strong evidence to support the impact of current smoking (Strietzel et al 2007).
- Diabetes (Daubert 2015).
- Host susceptibility to periodontitis/previous periodontitis. The study by Swierkot et al 2012 followed up non-periodontal and treated aggressive periodontitis patients for 5-16 years and the treated aggressive periodontitis patients had a 3.6x higher risk of mucositis, 14x higher risk of peri-implantitis, 4.4x higher risk of implant failure.
- Local factors – excess cement associated with signs of peri-implant disease in the majority of cases (81%). Some recent data suggest that cemented restorations may not be a problem if there is no excess cement, ie consider cemented with crevicular / supraginigval margins
- Limited data/no evidence that implant surface characteristics have a significant effect on initiation of peri-implantitis (Renvert 2009). However this does not mean that it does not have a role once problems have started.
4. Is keratinised tissue important around implants?
- Yes
- Warrer et al 1995 – ligated implant without keratinised mucosa had more recession and attachment loss.
- Schrott et al 2009 – implants with <2 mm of peri-implant keratinised mucosa were more prone to lingual plaque accumulation and bleeding as well as buccal soft-tissue recession over 5 years.
- Wennstrom & Derks 2012 – higher bleeding scores at implants with <2 mm keratinised mucosa.
5. What are the key points on management strategies?
- Preventive strategies – pick the right patient/site/implant, manage risk factors, place at the right time, place it in a restoratively driven manner, design your restoration for hygiene in advance and ensure systematic maintenance.
- When implant treatment is considered, patients should be informed on the risks for biological complications and the need for preventive care. An individual risk assessment should be performed and modifiable risk factors such as smoking should be eliminated. Treatment of periodontal disease aiming for elimination of residual pockets with bleeding on probing must precede implant placement.
- Since infection control is essential in the prevention of peri-implant diseases, patients should be instructed on personal oral hygiene with regular monitoring and reinforcement.
- Polish using a rubber cup. Antiseptics and chlorhexidine can be useful. Hand instruments and ultrasonics can be used for debridement. Mixed evidence for topical antimicrobials. Surgery usually required to treat peri-implantitis (resective/regenerative approach). We haven’t yet established predictable way to manage this condition.
- Maintenance and monitoring is critical as problems may still arise. During recall peri-implant tissues must be regularly examined including probing assessments with special emphasis on bleeding on probing. Intervals according to individual patient risk profile.
- Useful resource: http://prevention.efp.org/wp-content/uploads/2015/12/Prevention-of-peri-implant-diseases-guidance-for-dental-professionals.pdf
These notes were created following a webinar organised by the BSP.
To find out more about the BSP visit www.bsperio.org.uk
Learn more by reading some of our other articles here.



